CPAP machines are devices that play a crucial role in the treatment of sleep apnea. Sleep apnea is a sleep disorder characterized by pauses in breathing or shallow breaths during…
An In-depth Analysis of CPAP Machines and Functionality

latest techniques for sleep apnea therapy

CPAP machines are devices that play a crucial role in the treatment of sleep apnea. Sleep apnea is a sleep disorder characterized by pauses in breathing or shallow breaths during…
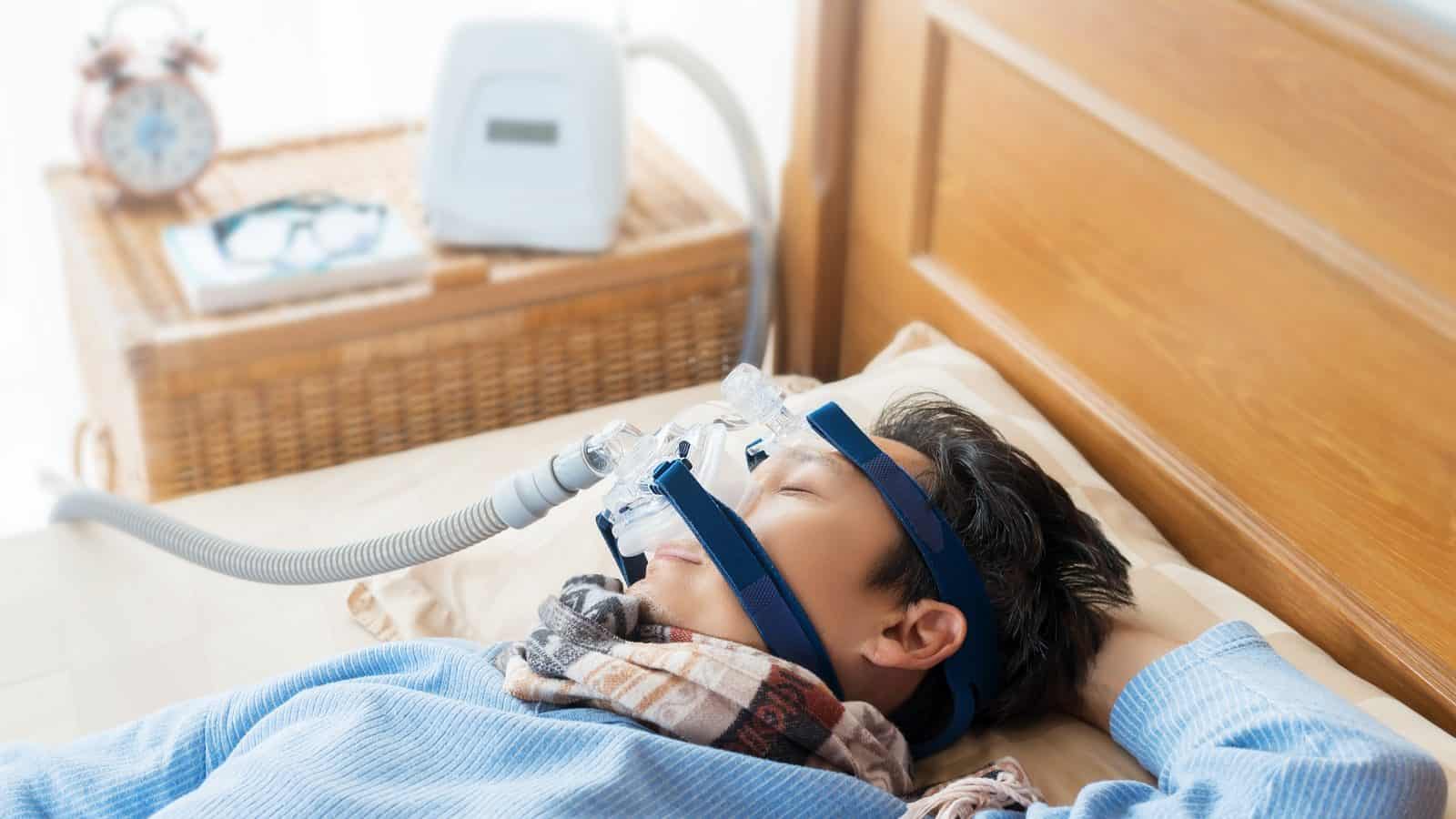
Sleep apnea is a prevalent sleep disorder that affects millions of people worldwide. With advancements in modern science, there has been a revolutionary change in the treatment options available for…

Sleep apnea is a common sleep disorder characterized by pauses in breathing or shallow breathing during sleep. It can significantly impact one's quality of life and overall health if left…

Sleep apnea is a sleep disorder that can be dangerous if left untreated. It can be divided into two main types - obstructive sleep apnea (OSA) and central sleep apnea…
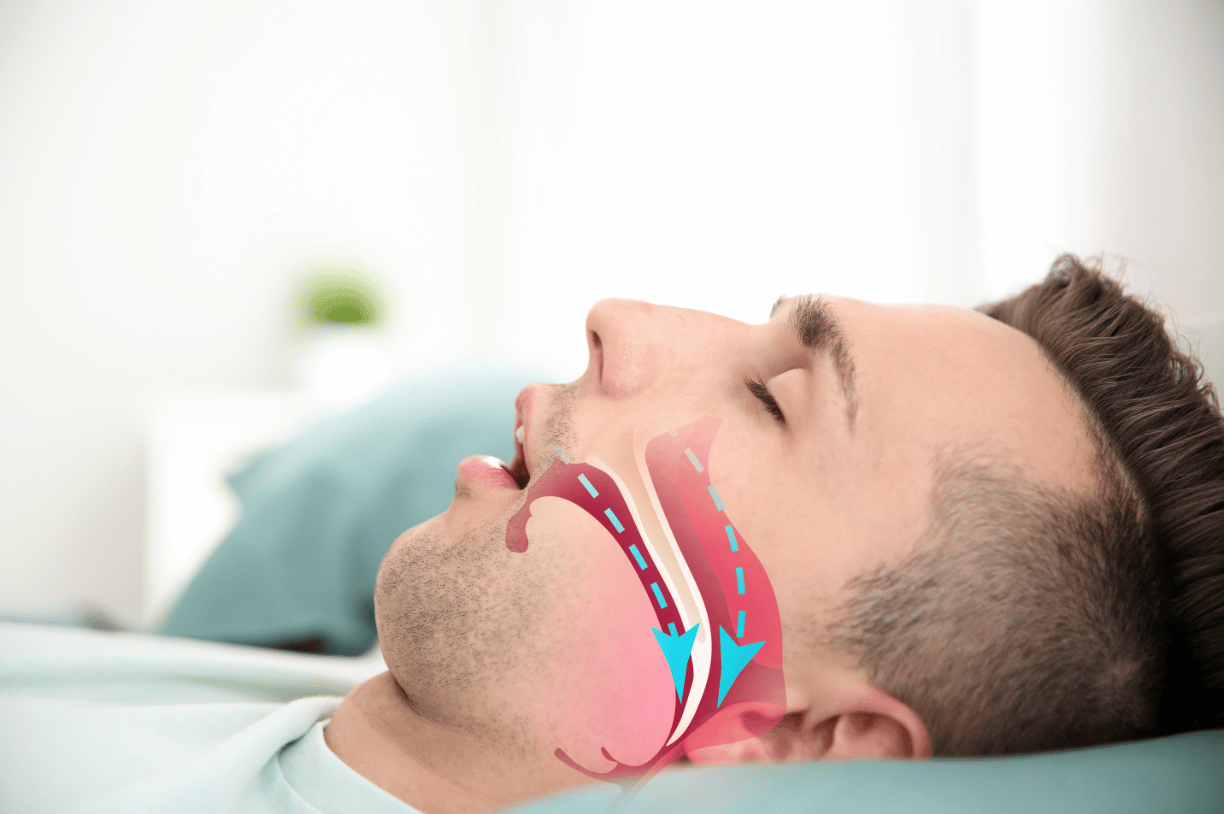
Snoring can be disruptive and make it difficult to get a good night's rest. Sleep Apnea is a serious sleep disorder that affects your breathing. It can be obstructive, central,…

If you suffer from obstructive sleep apnea, planning a short vacation can be quite challenging. Fortunately, Continuous Positive Airway Pressure (CPAP) therapy is a widely used and successful treatment. To…
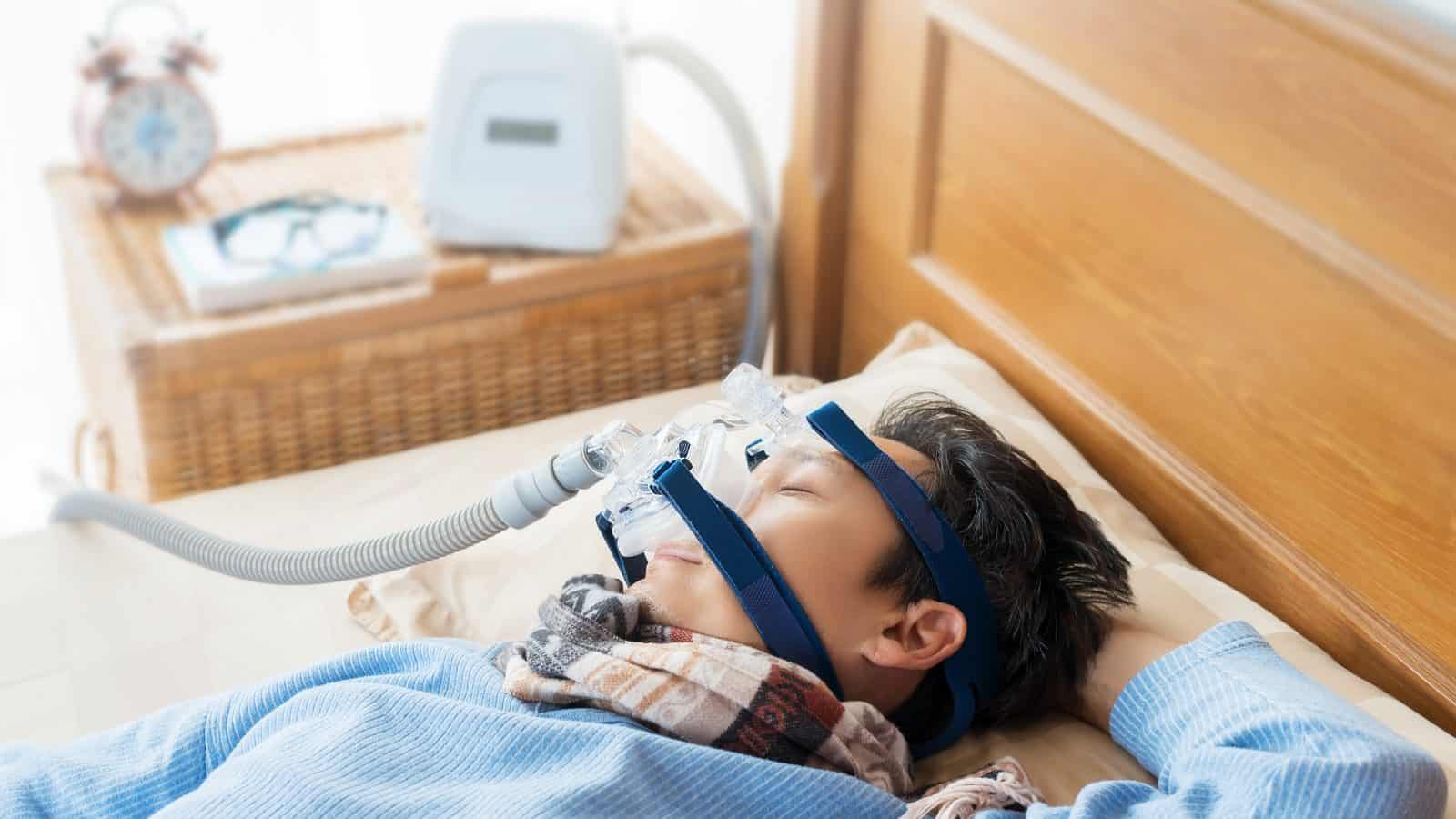
Many people suffer from severe obstructive sleep apnea (OSA) without knowing it. Interestingly, some people still don’t agree they are victims of the sleeping disorder even when they experience the…

Every year, millions of Australians are affected by sleep apnea. When you have this illness, you frequently stop breathing at night. Snoring is not a universal sign of sleep apnea,…

It could be challenging to adjust to CPAP machines treatment at first. The fact that many persons with sleep apnea detest their CPAP machines on their first usage may be…

Sixty percent of people with obstructive sleep apnea (OSA) also have GERD, suggesting a possible relationship between the two conditions. If you suffer with GERD, you know the agony may…